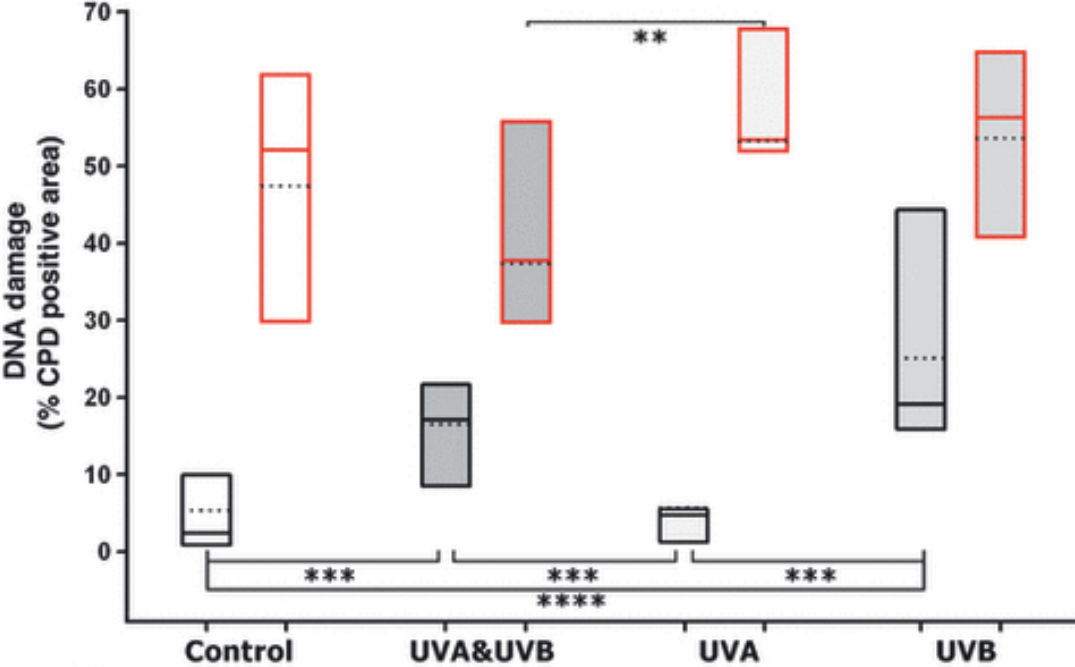
In his recent LessWrong post, Some takes on UV & cancer, Steve Byrnes comes out against the “Public Health Orthodoxy” on UV. Among other topics I won’t be addressing, Brynes claims that non-sunburn sun exposure does not increase risk of skin cancer, and suggests that people should aim to “wean off” sunscreen and develop a permanent tan.[1]Brynes is wrong and his advice is dangerous.Non-sunburn UV exposure causes cancerOur mechanistic understanding of UV-induced carcinogenesis is consistent with non-sunburn exposure causing cancerWe have a pretty solid understanding of how and why sun exposure causes cancer. UVB exposure causes direct DNA damage, whereas UVA causes damage primarily through oxidative stress.[2] Both of these pathways involve the formation of abnormal structures in DNA called photoproducts, such as cyclobutane pyrimidine dimers (CPDs). CPDs are a primary cause of melanoma.[3]CPDs do not require sunburn to form. For example, look at the second graph of Figure 4 of Miyamura et al. 2010, a small (n=7) study on the tanning process.[4] The black boxes show CPD presence after repeated sub-sunburn threshold UV exposure, designed to induce tanning. The red boxes show CPD presence after another exposure to 2 MED UV.[5] The overlap in the red boxes suggests that the protection offered by tanning is minimal: tanned skin still accumulates additional CPDs.In fact, tanning is caused by DNA damage, specifically the activity of the p53 tumor suppressor protein in response to UVB-induced damage.[6] This is why dermatologists say “there is no safe way to get a tan”: tanning requires exposing your skin to carcinogenic conditions.Sunscreen is effective at preventing CPD formation.[7] Contrary to Brynes’ claims that tans are “nature’s sunscreen” and “better than sunscreen,” you should still wear sunscreen if you have a tan.Empirical observations of indoor tanning provide evidence that non-sunburn exposure causes cancerIn the footnotes of his post, Brynes wrote, “I’m only talking about real sun-tans, not tanning beds, which I didn’t look into, they’re not my scene.” This is a confusing omission of a critical piece of evidence on the risks of tanning.Indoor tanning is robustly associated with higher risks of skin cancer, including melanoma. Ghiasvand et al. (2017), a prospective population study of 141,045 Norwegian women, found a dose-response relationship between indoor tanning use and melanoma risk, with the highest tertile of use sample having a 32% higher risk (8%-63% 95% CI) than the never use sample.[8] Gerami et al. (2025) compared around 3,000 dermatology patients that used indoor tanning with 3,000 age-matched controls, and found that tanning bed users were 2.85 times (2.0-3.99 95% CI) more likely to develop melanoma, with unique presentations indicative of a causal relationship with tanning bed use.[9]While indoor tanning can cause sunburn when used incorrectly, it is meant to induce tanning without sunburn. It’s implausible that the increased melanoma risk associated with tanning bed use is exclusively explained by sunburn. Tanning beds provide empirical evidence of large increases in melanoma risk from non-sunburn UV exposure.[10]Rebuttals to specific arguments from BrynesI’ve presented an independent case for why non-sunburn UV exposure is dangerous, and why a tan is not a good substitute for sunscreen. Now I’ll address the arguments Brynes made in favor of his claims.Sunscreen/cancer correlation studies do not control for sun exposure, but randomized trials support sunscreen useBrynes is skeptical that sunscreen prevents skin cancer, because correlation studies don’t find a link between sunscreen use and lower cancer rates.In particular, if sunlight-without-sunscreen causes deadly skin cancers, then why is the correlation between sunscreen use and deadly skin cancers so weak (after controlling for confounders like skin fairness and sun exposure)? This 2003 review found no effect, and neither did this 2018 review. (Indeed, the latter found a small, non-significant increase in skin cancer from sunscreen!)The studies in the linked reviews didn’t control for sun exposure, not really. Look at pages 5-11 of the 2018 review. Many of these studies did not even try to control for sun exposure, and those that tried used proxy variables such as “UVB intensity at site of residency”, “weeks spent every year in sunny resorts”, and/or asked for self-reported sun exposure. Due to these noisy or nonexistent controls, sunscreen use is likely still independently predictive of sun exposure in study populations.[11]It would be shocking if we got any usable information from correlation studies.There aren’t many good randomized trials on sunscreen. Research is made difficult due to poor application technique and adherence, the necessity of large cohorts with long follow-up times, and the fact that it’s hard to get funding for studies investigating settled questions. But we do have some.Green et al. (2011) conducted a 10-year study (n=1621) in Nambour, a town in Queensland, Australia. Participants were randomly assigned to daily or discretionary sunscreen application. After 10 years, 11 melanomas were found in the daily group and 22 in the discretionary group.[12]Skin color variation demonstrates strong evolutionary pressure to mitigate UV damageAlso, it’s worth noting that our ancestors have been outside all day every day for millions of years. So UV-induced health problems are only plausible if they’re pretty rare, mild, and/or late-in-life, albeit with some caveats.The evolutionary argument is weak to begin with. Melanoma, which makes up almost all deadly skin cancers, is indeed rare[13] and rarer among young people. Even if it weren’t, it’s not clear why we should expect evolution to have so thoroughly mitigated the problem that normal UV exposure is no longer harmful. The sun is a deadly laser, and evolving additional resistance against it would be costly. We evolved in an environment with teeth and sharp rocks, why isn’t our skin thick like a rhino?In this case, we actually have evidence there are strong evolutionary pressures towards mitigating UV-induced damage. As zebrask pointed out, skin color is highly correlated with UV exposure.Carcinogens rarely exhibit linear dose-response relationships, and occupational exposure data is hopelessly muddledBryes claims that occupational exposure is evidence against tans being dangerous.For example, there are people who work outside, without a shirt or sunscreen, basically all day every day for months on end. Maybe they have 50× more sun exposure than an office worker. Do they get 50× more skin cancer? No way. This would be a huge, easily-observable effect, and as far as I can tell, it has not been observed.In general, you should not expect linear dose-response relationships between carcinogen exposure and cancer risk. As an example to build intuition, the excess incidence of lung cancer in smokers is approximately “proportional to the fourth power of smoking duration multiplied by the number of cigarettes smoked per day.” The reasons why are complicated and depend heavily on the etiology of the cancer in question.The fact that people who get 50x more sun exposure than you don’t have 50x higher rates skin cancer does not mean your current level of sun exposure is not significantly contributing to your cancer risk.Do they get any more skin cancer than office workers? Maybe slightly—e.g. 20% more in this study of agricultural workers. Or, maybe not even slightly—there are enough confounders (e.g. sunburns, exposure to pesticide & fertilizers) that this little 20% effect might be unrelated to tans. So if sun-tans carry any cancer risk at all, I’m rounding it to zero.Brynes seems to have misread his cited study, which actually showed no increased risk for men and a 20% increased risk for women, who are probably not working shirtless, but it hardly matters. Gerami et al. (2025) included a passage relevant to Brynes’ argument.Moreover, the tanning industry has marketed the prevacation tan as a safe way to photoadapt skin in anticipation of recreational exposure, supported by observations that the relative risk of melanoma is higher in people who have a history of intermittent, blistering sunburns than in outdoor workers, and experiencing daily UV radiation. However, people who burn easily tend to avoid occupations with intense sun exposure, and most outdoor workers wear protective clothing over their trunk and upper extremities, where melanoma is most common.Brynes offered the confusing statement that because there are confounders, he is rounding 20% to zero. But confounders go both ways. The study could be vastly underestimating melanoma risk associated with agricultural work, for example because workers are physically healthier or of darker complexion than controls. The data is so noisy it’s close to useless for estimating the risks of tanning.ConclusionSubject-level takeawaysYou should wear sunscreen instead of trying to get a tan.Sun exposure is carcinogenic regardless of whether it causes sunburnsGetting a suntan requires exposure to carcinogenic damageHaving a tan does not fully protect you from further damageThat being said, I don’t necessarily endorse worrying much more about sun exposure than you currently do. Melanoma is rare, and dying of it is very rare. Touch grass, it’s good for you, and if you see a suspicious mole go see a dermatologist.Meta-level takeawaysHere are some principles I would endorse for reasoning better about cancer risk, and in general.[14]Prioritize mechanistic understandingThere is virtue in taking a bird’s-eye-view of a phenomenon, especially poorly understood ones, but understanding is incomplete without a bottom-up mechanistic model. We have heaps of research addressing UV-induced carcinogenesis, all of which points to sunburns not being required for carcinogenic damage. Brynes’ post skipped engaging with this research entirely.Beware the streetlight effectBrynes never disputed the claim that sunburns are linked to cancer risk, probably because of the abundance of robust data showing this fact. This data arises from the fact that studies in this field often ask about sunburns as a proxy for sun exposure. People are much more likely to accurately recall getting sunburned, than they are to recall how tanned they were, or how many hours they spent in the sun. The link between non-sunburn exposure and cancer is intrinsically harder to accurately investigate than the link between sunburn and cancer. Byrnes should have accounted for this when comparing the relative quality of the data supporting each claim, instead of accepting studies presenting extremely noisy data as evidence of absence.The orthodoxy is usually rightMainstream expert consensus is often oversimplified, but only occasionally wrong. People who hang out in contrarian circles are disproportionately exposed to the rare circumstances where mainstream consensus is the most dubious. Don’t overindex on exceptions to the rule. If you ever find yourself disagreeing with the expert consensus about a topic outside your own expertise, you should have strong priors that you are wrong.[15]^Brynes disclaimed his post with, “I certainly wouldn’t suggest that readers make health decisions based on poorly-researched contrarian blog posts by randos on the internet.”^Sample A, He YY. Mechanisms and prevention of UV-induced melanoma. Photodermatol Photoimmunol Photomed. 2018 Jan;34(1):13-24. doi: 10.1111/phpp.12329. Epub 2017 Aug 2. PMID: 28703311; PMCID: PMC5760354.Check out Figure 1 and Figure 2 for a more detailed overview on the pathways of UV carcinogenesis. Cancer is complicated, and I’m giving a 101 summary only. ^Why do we know this? Many reasons. Skin-cancer related mutations in the p53 tumor suppressor gene occur in the same locations that UVB causes CPDs, and mutations in melanoma in general are the same kinds that occur downstream of CPDs. The genetic disorder xeroderma pigmentosum, involving deficiencies in the CPD (and other photoproduct) repair pathway, causes a 1000x increase in the risk of melanoma.CPD formation is not the only mechanism by which UV light can cause cancer, but it is an important pathway. In general, DNA damage of any kind is not the only mechanism by which something can increase your risk of cancer, many carcinogens are not mutagens.^Miyamura, Y., Coelho, S.G., Schlenz, K., Batzer, J., Smuda, C., Choi, W., Brenner, M., Passeron, T., Zhang, G., Kolbe, L., Wolber, R. and Hearing, V.J. (2011), The deceptive nature of UVA tanning versus the modest protective effects of UVB tanning on human skin. Pigment Cell & Melanoma Research, 24: 136-147. https://doi.org/10.1111/j.1755-148X.2010.00764.xIt’s a small study (n=7), though it has the advantage that each participant participated in every protocol by using different patches of skin. Still, interpret specific results cautiously. I’m confident of the important claims I’m making using this study, and if anyone doubts me, I can find better data.^MED is the lowest dose that causes reddening of the skin, a set dose determined for each participant before the study.^Videira IF, Moura DF, Magina S. Mechanisms regulating melanogenesis. An Bras Dermatol. 2013 Jan-Feb;88(1):76-83. doi: 10.1590/s0365-05962013000100009. PMID: 23539007; PMCID: PMC3699939.See the paragraph with “….suggested for the first time a cause-effect relation between DNA damage and melanogenesis” under “Extrinsic regulation of skin pigmentation by ultraviolet radiation (UVR)” for an overview with useful links.^Young AR, Greenaway J, Harrison GI, Lawrence KP, Sarkany R, Douki T, Boyer F, Josse G, Questel E, Monteil C, Rossi AB. Sub-optimal Application of a High SPF Sunscreen Prevents Epidermal DNA Damage in Vivo. Acta Derm Venereol. 2018 Oct 10;98(9):880-887. doi: 10.2340/00015555-2992. PMID: 29944164.See Figures 3 or 4, and note that this paper involved exposure to much higher doses of UV (30 MED versus 2 MED) than Miyamura et al. I couldn’t easily find a 1:1 comparison between sunscreen and tanning to definitively claim that sunscreen is more protective than a tan. However, as the protection from sunscreen stacks with protection from a tan and does not require you to first accumulate DNA damage, I can still confidently recommend sunscreen.^Reza Ghiasvand, Corina S. Rueegg, Elisabete Weiderpass, Adele C. Green, Eiliv Lund, Marit B. Veierød, Indoor Tanning and Melanoma Risk: Long-Term Evidence From a Prospective Population-Based Cohort Study, American Journal of Epidemiology, Volume 185, Issue 3, 1 February 2017, Pages 147–156, https://doi.org/10.1093/aje/kww148You should be cautious about inferring causality from cohort studies. In this case, based on the overall literature, I’m highly confident that indoor tanning causes melanoma.^Pedram Gerami et al., Molecular effects of indoor tanning. Sci. Adv. 11, eady4878 (2025). DOI:10.1126/sciadv.ady4878^Is it possible that sunlight is fine but indoor tanning lights aren’t? To quote Gerami et al. (2025), “The tanning bed industry argues that indoor tanning is safer than natural sunlight because UVB is more mutagenic than UVA; however, the absolute irradiance of tanning beds and outdoor sunlight is similar in the UVB range and 10 to 15 times higher in the UVA range than outdoor sunlight.” I suspect these figures likely differ by model. UVB exposure is the most important factor; I find it plausible that tanning beds are either somewhat more or somewhat less dangerous than sunlight, but not that tanning beds are dangerous and sunlight is totally fine.^Imagine you know Person A and Person B live in San Francisco, vacation in the Bahamas for 2 weeks a year, and reported 4 hours of average daily sun exposure. You also know that Person A uses more sunscreen. You have to place a bet on whether Person A or Person B is exposed to more UV light.You’d still give good odds on A, right?^Green AC, Williams GM, Logan V, Strutton GM. Reduced melanoma after regular sunscreen use: randomized trial follow-up. J Clin Oncol. 2011 Jan 20;29(3):257-63. doi: 10.1200/JCO.2010.28.7078. Epub 2010 Dec 6. PMID: 21135266.^The lifetime incidence of melanoma in 3% for white Americans and 0.1% for black Americans, 2.6% for British people of any ethnicity, and 5.4% for Australians of any ethnicity. No points for guessing why these numbers are different.^I didn’t know how to phrase this in a way that didn’t sound rude to Brynes, since I am criticizing his reasoning process. Brynes, if you’re reading this, I hope you take my post in the constructive manner it was intended.^Brynes did understand this, to his credit:This is “strong opinions, weakly held”. Even I myself am too nervous to fully act on these opinions; instead I kinda split the difference between Public Health Orthodoxy and what I actually believe. But I would go further than he did, and endorse not believing something until you can support it with more confidence.Discuss Read More
Contra Byrnes on UV & Cancer
In his recent LessWrong post, Some takes on UV & cancer, Steve Byrnes comes out against the “Public Health Orthodoxy” on UV. Among other topics I won’t be addressing, Brynes claims that non-sunburn sun exposure does not increase risk of skin cancer, and suggests that people should aim to “wean off” sunscreen and develop a permanent tan.[1]Brynes is wrong and his advice is dangerous.Non-sunburn UV exposure causes cancerOur mechanistic understanding of UV-induced carcinogenesis is consistent with non-sunburn exposure causing cancerWe have a pretty solid understanding of how and why sun exposure causes cancer. UVB exposure causes direct DNA damage, whereas UVA causes damage primarily through oxidative stress.[2] Both of these pathways involve the formation of abnormal structures in DNA called photoproducts, such as cyclobutane pyrimidine dimers (CPDs). CPDs are a primary cause of melanoma.[3]CPDs do not require sunburn to form. For example, look at the second graph of Figure 4 of Miyamura et al. 2010, a small (n=7) study on the tanning process.[4] The black boxes show CPD presence after repeated sub-sunburn threshold UV exposure, designed to induce tanning. The red boxes show CPD presence after another exposure to 2 MED UV.[5] The overlap in the red boxes suggests that the protection offered by tanning is minimal: tanned skin still accumulates additional CPDs.In fact, tanning is caused by DNA damage, specifically the activity of the p53 tumor suppressor protein in response to UVB-induced damage.[6] This is why dermatologists say “there is no safe way to get a tan”: tanning requires exposing your skin to carcinogenic conditions.Sunscreen is effective at preventing CPD formation.[7] Contrary to Brynes’ claims that tans are “nature’s sunscreen” and “better than sunscreen,” you should still wear sunscreen if you have a tan.Empirical observations of indoor tanning provide evidence that non-sunburn exposure causes cancerIn the footnotes of his post, Brynes wrote, “I’m only talking about real sun-tans, not tanning beds, which I didn’t look into, they’re not my scene.” This is a confusing omission of a critical piece of evidence on the risks of tanning.Indoor tanning is robustly associated with higher risks of skin cancer, including melanoma. Ghiasvand et al. (2017), a prospective population study of 141,045 Norwegian women, found a dose-response relationship between indoor tanning use and melanoma risk, with the highest tertile of use sample having a 32% higher risk (8%-63% 95% CI) than the never use sample.[8] Gerami et al. (2025) compared around 3,000 dermatology patients that used indoor tanning with 3,000 age-matched controls, and found that tanning bed users were 2.85 times (2.0-3.99 95% CI) more likely to develop melanoma, with unique presentations indicative of a causal relationship with tanning bed use.[9]While indoor tanning can cause sunburn when used incorrectly, it is meant to induce tanning without sunburn. It’s implausible that the increased melanoma risk associated with tanning bed use is exclusively explained by sunburn. Tanning beds provide empirical evidence of large increases in melanoma risk from non-sunburn UV exposure.[10]Rebuttals to specific arguments from BrynesI’ve presented an independent case for why non-sunburn UV exposure is dangerous, and why a tan is not a good substitute for sunscreen. Now I’ll address the arguments Brynes made in favor of his claims.Sunscreen/cancer correlation studies do not control for sun exposure, but randomized trials support sunscreen useBrynes is skeptical that sunscreen prevents skin cancer, because correlation studies don’t find a link between sunscreen use and lower cancer rates.In particular, if sunlight-without-sunscreen causes deadly skin cancers, then why is the correlation between sunscreen use and deadly skin cancers so weak (after controlling for confounders like skin fairness and sun exposure)? This 2003 review found no effect, and neither did this 2018 review. (Indeed, the latter found a small, non-significant increase in skin cancer from sunscreen!)The studies in the linked reviews didn’t control for sun exposure, not really. Look at pages 5-11 of the 2018 review. Many of these studies did not even try to control for sun exposure, and those that tried used proxy variables such as “UVB intensity at site of residency”, “weeks spent every year in sunny resorts”, and/or asked for self-reported sun exposure. Due to these noisy or nonexistent controls, sunscreen use is likely still independently predictive of sun exposure in study populations.[11]It would be shocking if we got any usable information from correlation studies.There aren’t many good randomized trials on sunscreen. Research is made difficult due to poor application technique and adherence, the necessity of large cohorts with long follow-up times, and the fact that it’s hard to get funding for studies investigating settled questions. But we do have some.Green et al. (2011) conducted a 10-year study (n=1621) in Nambour, a town in Queensland, Australia. Participants were randomly assigned to daily or discretionary sunscreen application. After 10 years, 11 melanomas were found in the daily group and 22 in the discretionary group.[12]Skin color variation demonstrates strong evolutionary pressure to mitigate UV damageAlso, it’s worth noting that our ancestors have been outside all day every day for millions of years. So UV-induced health problems are only plausible if they’re pretty rare, mild, and/or late-in-life, albeit with some caveats.The evolutionary argument is weak to begin with. Melanoma, which makes up almost all deadly skin cancers, is indeed rare[13] and rarer among young people. Even if it weren’t, it’s not clear why we should expect evolution to have so thoroughly mitigated the problem that normal UV exposure is no longer harmful. The sun is a deadly laser, and evolving additional resistance against it would be costly. We evolved in an environment with teeth and sharp rocks, why isn’t our skin thick like a rhino?In this case, we actually have evidence there are strong evolutionary pressures towards mitigating UV-induced damage. As zebrask pointed out, skin color is highly correlated with UV exposure.Carcinogens rarely exhibit linear dose-response relationships, and occupational exposure data is hopelessly muddledBryes claims that occupational exposure is evidence against tans being dangerous.For example, there are people who work outside, without a shirt or sunscreen, basically all day every day for months on end. Maybe they have 50× more sun exposure than an office worker. Do they get 50× more skin cancer? No way. This would be a huge, easily-observable effect, and as far as I can tell, it has not been observed.In general, you should not expect linear dose-response relationships between carcinogen exposure and cancer risk. As an example to build intuition, the excess incidence of lung cancer in smokers is approximately “proportional to the fourth power of smoking duration multiplied by the number of cigarettes smoked per day.” The reasons why are complicated and depend heavily on the etiology of the cancer in question.The fact that people who get 50x more sun exposure than you don’t have 50x higher rates skin cancer does not mean your current level of sun exposure is not significantly contributing to your cancer risk.Do they get any more skin cancer than office workers? Maybe slightly—e.g. 20% more in this study of agricultural workers. Or, maybe not even slightly—there are enough confounders (e.g. sunburns, exposure to pesticide & fertilizers) that this little 20% effect might be unrelated to tans. So if sun-tans carry any cancer risk at all, I’m rounding it to zero.Brynes seems to have misread his cited study, which actually showed no increased risk for men and a 20% increased risk for women, who are probably not working shirtless, but it hardly matters. Gerami et al. (2025) included a passage relevant to Brynes’ argument.Moreover, the tanning industry has marketed the prevacation tan as a safe way to photoadapt skin in anticipation of recreational exposure, supported by observations that the relative risk of melanoma is higher in people who have a history of intermittent, blistering sunburns than in outdoor workers, and experiencing daily UV radiation. However, people who burn easily tend to avoid occupations with intense sun exposure, and most outdoor workers wear protective clothing over their trunk and upper extremities, where melanoma is most common.Brynes offered the confusing statement that because there are confounders, he is rounding 20% to zero. But confounders go both ways. The study could be vastly underestimating melanoma risk associated with agricultural work, for example because workers are physically healthier or of darker complexion than controls. The data is so noisy it’s close to useless for estimating the risks of tanning.ConclusionSubject-level takeawaysYou should wear sunscreen instead of trying to get a tan.Sun exposure is carcinogenic regardless of whether it causes sunburnsGetting a suntan requires exposure to carcinogenic damageHaving a tan does not fully protect you from further damageThat being said, I don’t necessarily endorse worrying much more about sun exposure than you currently do. Melanoma is rare, and dying of it is very rare. Touch grass, it’s good for you, and if you see a suspicious mole go see a dermatologist.Meta-level takeawaysHere are some principles I would endorse for reasoning better about cancer risk, and in general.[14]Prioritize mechanistic understandingThere is virtue in taking a bird’s-eye-view of a phenomenon, especially poorly understood ones, but understanding is incomplete without a bottom-up mechanistic model. We have heaps of research addressing UV-induced carcinogenesis, all of which points to sunburns not being required for carcinogenic damage. Brynes’ post skipped engaging with this research entirely.Beware the streetlight effectBrynes never disputed the claim that sunburns are linked to cancer risk, probably because of the abundance of robust data showing this fact. This data arises from the fact that studies in this field often ask about sunburns as a proxy for sun exposure. People are much more likely to accurately recall getting sunburned, than they are to recall how tanned they were, or how many hours they spent in the sun. The link between non-sunburn exposure and cancer is intrinsically harder to accurately investigate than the link between sunburn and cancer. Byrnes should have accounted for this when comparing the relative quality of the data supporting each claim, instead of accepting studies presenting extremely noisy data as evidence of absence.The orthodoxy is usually rightMainstream expert consensus is often oversimplified, but only occasionally wrong. People who hang out in contrarian circles are disproportionately exposed to the rare circumstances where mainstream consensus is the most dubious. Don’t overindex on exceptions to the rule. If you ever find yourself disagreeing with the expert consensus about a topic outside your own expertise, you should have strong priors that you are wrong.[15]^Brynes disclaimed his post with, “I certainly wouldn’t suggest that readers make health decisions based on poorly-researched contrarian blog posts by randos on the internet.”^Sample A, He YY. Mechanisms and prevention of UV-induced melanoma. Photodermatol Photoimmunol Photomed. 2018 Jan;34(1):13-24. doi: 10.1111/phpp.12329. Epub 2017 Aug 2. PMID: 28703311; PMCID: PMC5760354.Check out Figure 1 and Figure 2 for a more detailed overview on the pathways of UV carcinogenesis. Cancer is complicated, and I’m giving a 101 summary only. ^Why do we know this? Many reasons. Skin-cancer related mutations in the p53 tumor suppressor gene occur in the same locations that UVB causes CPDs, and mutations in melanoma in general are the same kinds that occur downstream of CPDs. The genetic disorder xeroderma pigmentosum, involving deficiencies in the CPD (and other photoproduct) repair pathway, causes a 1000x increase in the risk of melanoma.CPD formation is not the only mechanism by which UV light can cause cancer, but it is an important pathway. In general, DNA damage of any kind is not the only mechanism by which something can increase your risk of cancer, many carcinogens are not mutagens.^Miyamura, Y., Coelho, S.G., Schlenz, K., Batzer, J., Smuda, C., Choi, W., Brenner, M., Passeron, T., Zhang, G., Kolbe, L., Wolber, R. and Hearing, V.J. (2011), The deceptive nature of UVA tanning versus the modest protective effects of UVB tanning on human skin. Pigment Cell & Melanoma Research, 24: 136-147. https://doi.org/10.1111/j.1755-148X.2010.00764.xIt’s a small study (n=7), though it has the advantage that each participant participated in every protocol by using different patches of skin. Still, interpret specific results cautiously. I’m confident of the important claims I’m making using this study, and if anyone doubts me, I can find better data.^MED is the lowest dose that causes reddening of the skin, a set dose determined for each participant before the study.^Videira IF, Moura DF, Magina S. Mechanisms regulating melanogenesis. An Bras Dermatol. 2013 Jan-Feb;88(1):76-83. doi: 10.1590/s0365-05962013000100009. PMID: 23539007; PMCID: PMC3699939.See the paragraph with “….suggested for the first time a cause-effect relation between DNA damage and melanogenesis” under “Extrinsic regulation of skin pigmentation by ultraviolet radiation (UVR)” for an overview with useful links.^Young AR, Greenaway J, Harrison GI, Lawrence KP, Sarkany R, Douki T, Boyer F, Josse G, Questel E, Monteil C, Rossi AB. Sub-optimal Application of a High SPF Sunscreen Prevents Epidermal DNA Damage in Vivo. Acta Derm Venereol. 2018 Oct 10;98(9):880-887. doi: 10.2340/00015555-2992. PMID: 29944164.See Figures 3 or 4, and note that this paper involved exposure to much higher doses of UV (30 MED versus 2 MED) than Miyamura et al. I couldn’t easily find a 1:1 comparison between sunscreen and tanning to definitively claim that sunscreen is more protective than a tan. However, as the protection from sunscreen stacks with protection from a tan and does not require you to first accumulate DNA damage, I can still confidently recommend sunscreen.^Reza Ghiasvand, Corina S. Rueegg, Elisabete Weiderpass, Adele C. Green, Eiliv Lund, Marit B. Veierød, Indoor Tanning and Melanoma Risk: Long-Term Evidence From a Prospective Population-Based Cohort Study, American Journal of Epidemiology, Volume 185, Issue 3, 1 February 2017, Pages 147–156, https://doi.org/10.1093/aje/kww148You should be cautious about inferring causality from cohort studies. In this case, based on the overall literature, I’m highly confident that indoor tanning causes melanoma.^Pedram Gerami et al., Molecular effects of indoor tanning. Sci. Adv. 11, eady4878 (2025). DOI:10.1126/sciadv.ady4878^Is it possible that sunlight is fine but indoor tanning lights aren’t? To quote Gerami et al. (2025), “The tanning bed industry argues that indoor tanning is safer than natural sunlight because UVB is more mutagenic than UVA; however, the absolute irradiance of tanning beds and outdoor sunlight is similar in the UVB range and 10 to 15 times higher in the UVA range than outdoor sunlight.” I suspect these figures likely differ by model. UVB exposure is the most important factor; I find it plausible that tanning beds are either somewhat more or somewhat less dangerous than sunlight, but not that tanning beds are dangerous and sunlight is totally fine.^Imagine you know Person A and Person B live in San Francisco, vacation in the Bahamas for 2 weeks a year, and reported 4 hours of average daily sun exposure. You also know that Person A uses more sunscreen. You have to place a bet on whether Person A or Person B is exposed to more UV light.You’d still give good odds on A, right?^Green AC, Williams GM, Logan V, Strutton GM. Reduced melanoma after regular sunscreen use: randomized trial follow-up. J Clin Oncol. 2011 Jan 20;29(3):257-63. doi: 10.1200/JCO.2010.28.7078. Epub 2010 Dec 6. PMID: 21135266.^The lifetime incidence of melanoma in 3% for white Americans and 0.1% for black Americans, 2.6% for British people of any ethnicity, and 5.4% for Australians of any ethnicity. No points for guessing why these numbers are different.^I didn’t know how to phrase this in a way that didn’t sound rude to Brynes, since I am criticizing his reasoning process. Brynes, if you’re reading this, I hope you take my post in the constructive manner it was intended.^Brynes did understand this, to his credit:This is “strong opinions, weakly held”. Even I myself am too nervous to fully act on these opinions; instead I kinda split the difference between Public Health Orthodoxy and what I actually believe. But I would go further than he did, and endorse not believing something until you can support it with more confidence.Discuss Read More